Revision Rhinoplasty
What is revision rhinoplasty?
Revision rhinoplasty is additional surgery to a nose that has already had at least one rhinoplasty surgery. It can be a second surgery performed by the same surgeon after the first surgery did not heal as expected, or performed by another surgeon different from the first surgeon.
The risk of needing a revision after a primary rhinoplasty is what defines a particular surgeon’s revision rate. The rhinoplasty revision rate within the U.S. varies from 4% to 20%. At Westlake Dermatology, our plastic surgeons’ revision rates are all under 5%.
Before and After Revision Rhinoplasty
View Revision Rhinoplasty Photo Gallery
How is revision rhinoplasty different than primary rhinoplasty?
Revision rhinoplasty does not specify how many previous rhinoplasties someone has had. Regardless of whether the patient only had one previous rhinoplasty or ten, it’s still called a revision rhinoplasty.
Each time any part of the body is operated upon, the area heals by forming scar tissue. Even after one successful rhinoplasty, scar tissue has formed. With each additional rhinoplasty, more and more scar tissue forms. This makes the healing less predictable with each surgery.
Rhinoplasty also weakens nasal tissues, so the surgeon must rebuild the weak areas with new structural grafting using cartilage from the septum, ear or rib. Each time a rhinoplasty is performed on the same nose, more unpredictability and weakening can result, so more structural grafting is required, making the risk of even more revisions higher. The risk of requiring yet another revision after one revision runs between 15% and 50% in the U.S., even by the most skilled surgeons. At Westlake Dermatology, fortunately we have very experienced surgeons whose revision rates are at the lowest end of this spectrum.
Revision rhinoplasty usually takes longer than primary rhinoplasty (except if the revision is a minor touch-up due to a small irregularity or asymmetry). This is because the scar tissue that has formed requires the surgeon to slow down his dissection lest he do more damage, and then harvest cartilage from areas outside of the nose. The scarred tissues have been weakened and/or damaged by the first surgery (so are difficult to re-contour and support), requiring careful repair by rebuilding their contours and strength. Surgical times for complicated revisions can vary from 3 hours to 6 hours or more.
Do I need a revision rhinoplasty?
If you have had a primary rhinoplasty and are unhappy with the outcome, speak to your surgeon first. If it is something minor that does not affect your overall looks, then you and your surgeon must carefully weigh the risks of revision against the benefits of a minor improvement. If, on the other hand, you have a significant deformity and/or worsened nasal obstruction (a botched nose), then a revision rhinoplasty may be the best option.
Look at your before-and-after pictures and ask yourself:
- Do I look better overall than I did before my previous rhinoplasty? If so, are the risks of a revision worth the improvement? If not, will changing the nose further make me happy?
- How is my breathing compared to before surgery? If it is worse, can more surgery improve it?
Photo-imaging is an invaluable tool that can help you and your surgeon answer some of these questions. By morphing your photos with your surgeon, you can better explain what you see as the problems, and he/she can show you how revision rhinoplasty can correct these problems and what the limitations are of the surgery. Photo-imaging is a critical step in planning for successful revision rhinoplasty.
What are the risks and complications of revision rhinoplasty?
The risks of revision rhinoplasty are similar to those of primary rhinoplasty. There are short term risks and long term risks.
Short term risks include:
- Infection
- Severe bleeding
- Hematoma
- Risks of general anesthesia
Long term risks include:
- Poor outcome aesthetically
- Continued nasal obstruction including septal perforation
- Scarring
- Deformity requiring yet another surgery
When discussing revision rhinoplasty with your surgeon, make sure you are provided an estimation of what your chances are for a good result and if your nose presents any particular challenges or risks. Remember that even in the best of hands, the chance of needing yet another revision is still 15%.
How is revision rhinoplasty performed?
The types of incisions and the surgery is performed is called the “surgical approach”. Each surgeon chooses their approach based upon the complexity of the individual surgery and the best results that can be achieved with the chosen approach. The most common approach utilized for revision rhinoplasty is the open, or external, rhinoplasty approach.
During an open rhinoplasty, an incision is made in the columella, between the two nostrils, and is carried into incisions along the nostril edges. This approach has the advantage of being able to expose the entire external anatomy of the tip and bridge and can be modified based upon the amount of exposure needed for a particular patient. Also with this approach, any septal straightening and valve repair is much easier because the view is more complete of these important areas. The only downside of the open approach is the small scar left in the columella. Some surgeons argue that the open approach causes more swelling, but most experienced open rhinoplasty surgeons do not see this in their patients’ recoveries.
Once the nose has been opened, deformities can be corrected, deviations repaired and weaknesses strengthened. Today’s revision rhinoplasty is much different than that employed by surgeons of the past. Preservation of strength and structure is emphasized. If weaknesses exist, they are strengthened with a combination of suture techniques and structural grafting. Grafts ideally come from your own cartilage, either from the septum, ear or rib.
Here is a summary of the pros and cons of each grafting type:
- Septal cartilage
- Pros: Strong cartilage that is the ideal thickness for structural grafting, providing strength without too much bulk.
- Cons: Some septal cartilage is not straight enough, strong enough or plentiful enough to use for all grafting needs. This is particularly true when previous septoplasty has been performed, or if a nose is naturally small.
- Ear (conchal) cartilage
- Pros: Ear cartilage is harvested from the concha, or bowl, of the ear so does not change the ear’s appearance. It is excellent for grafting that is not load bearing (such as in spreader grafting). It is soft and pliable, so excellent for filling irregularities and depressions.
- Cons: Since it is softer and more curved than septal cartilage, it must be doubled up to use for load bearing, such as when supporting a droopy tip as a strut graft. It also required healing from a 2nd area outside of the nose.
- Rib (costal) cartilage
- Pros: Rib cartilage is strong and plentiful, so ideal in revision cases when a large amount of strong grafting is required.
- Cons: Technically more difficult to harvest than ear, with a longer recovery. During harvest there is the risk of pneumothorax, or a collapsed lung, although this risk is rare in experienced hands. The cartilage is thick, so cutting it into thin strips is required so that excess bulk is not added to the nose. However, thin strips can warp over time, the main problem with rib cartilage. Older patients may have rib cartilage that has ossified, or turned to bone, making it unusable for grafting.
- Cadaver rib cartilage
- Pros: All the benefits of your own rib cartilage, without the need for harvesting from your own rib. No risk of ossification.
- Cons: Unlike your own cartilage, which a living tissue that continues to live when transplanted into your nose, this is dead tissue. It does not form its own blood supply, so may be less reliable as the years pass. For this reason, many surgeons prefer it only for older patients.
- Alloplasts (artificial implants)
- Pros: Readily available, and of a variety of materials.
- Cons: Infection rates can exceed 5% and risk of infection is life-long. If infected, the implant must be removed, potentially requiring an entirely new revision with much more scar due to the infection. Very few surgeons use alloplasts today in revision rhinoplasty.
Common grafts placed during revision rhinoplasty are similar to those placed in primary rhinoplasty:
- Spreader grafts: Placed between the dorsal septum and upper lateral cartilages to open and stiffen the internal nasal valves
- Columellar strut graft: Placed in a pocket between the medial crura in the columella to support the tip
- Septal extension graft: Extends the length of the septum so it ends between the medial crura. The medial crura are then sewn to it in a tongue-in-groove fashion, providing a strong anchor to stabilize the tip.
- Rim graft: Placed in a pocket along the rim of the nostril to stabilize the nostril and support the external nasal valve
- Alar batten graft: Placed on top of the lateral crus to support a weak nasal sidewall and support the internal nasal valve
- Lateral crural strut graft: Placed beneath the lateral crus to flatten and support it, improving the internal nasal valve
- Tip graft: Placed on top of the tip cartilages centrally to create projection and definition
- Dorsal onlay graft: Placed on the bridge to raise its height
Not all revision rhinoplasties require all these grafts, but most require many of them.
What is healing like after revision rhinoplasty?
Revision rhinoplasty takes about 50% longer than primary rhinoplasty at each stage of healing.
Stage 1: Immediately after surgery through 7 days
- Pain: Pain varies significantly between patients. On the 0-to-10 point pain index, where 10 is the worst pain ever, most patients rate their pain between 4 and 8. We employ many strategies to control pain and try to avoid narcotic use. Lots of ice around the nose and eyes really helps. All patients receive celeocoxib (Celebrex) before and after surgery. This is a non-steroidal anti-inflammatory drug (NSAID) that does not increase postoperative bleeding but improves pain. All patients also receive a narcotic to use for severe pain (higher than 7 on the pain index. Most patients use some narcotic during the first few days, when pain is at its worst.
- Bleeding: Since we do not use postoperative packing, the nose will bleed for the first night after surgery. By the day after surgery, most bleeding stops.
- Swelling/ Bruising: This varies by patient and peaks by 72 hours after surgery. Using ice, elevating your head and taking Arnica montana really helps to minimize bruising and lessen swelling.
- Breathing: Severe nasal obstruction occurs after surgery due to swelling. By 4 to 5 days after surgery the swelling inside the nose has started to diminish so some air flow is possible. Using saline spray and Afrin decongestant spray at night for the first week helps to keep the nose clearer.
- Cast/ Sutures: These are removed after one week.
- What are my dos and don’ts?
- Do use lots of ice, keep your head elevated higher than your heart, minimize narcotic use by taking Celebrex around the clock and do not overexert yourself.
- Don’t blow your nose, get your cast wet, or take narcotics to prevent pain (you may not have any). Don’t fixate on how your nose looks: swelling distorts the appearance of the nose.
- Take supplements that help with healing, like Arnica and topical anti-bruising creams (Arnica cream, Vitamin K cream). We like Mend, a nutritional supplement that improves Stage 1 and Stage 2 healing.
Stage 2: One week to one month after surgery
- Swelling: Initial swelling will start to come down, but soon the nose enters the contraction phase of healing, where it becomes firmer. As one area stays swollen and another improves, the nose can start to look asymmetric. This is a normal part of healing. Nostril shape especially can look funny as contraction occurs. This is a normal part of healing and will soon subside. Your smile will also look stiff and funny until swelling has diminished. Depending on how your swelling is resolving, in rare cases you may be advised to tape your nose to help the swelling come down faster.
- Numbness/ Stiffness: This is normal and can take many months to disappear.
- Breathing: Airflow improves during the first month of healing. However, it can take up to six months for airflow to return completely to normal.
- What are my dos and don’ts?
- You may begin to exercise as long as it does not make swelling worse. You may wear glasses/ sunglasses/masks. Apply warm compresses to any residual bruises. You may swim and fly after two weeks.
- Do not engage in any activity that puts your nose at risk of getting hit (sports, horseplay, crowded events, drinking excessively). Do not get your nose sunburned.
- Scar gels may be used to improve the appearance of any external incisions.
Stage 3: One month to three months after surgery
- Swelling: Continue taping if needed. If swelling persists, especially with thicker skin or previous scarring, triamcinolone (Kenalog) and fluorouracil may be injected into the tip area to improve it faster. Prolonged swelling can interfere with your final result when it turns to scar.
- Breathing: Continued improvement as swelling decreases and nasal mucous production returns to normal.
- What are my dos and don’ts?
- You may SCUBA and engage in contact sports after 2 months. Remember if your nose breaks, repair will be even more difficult after revision rhinoplasty.
- Lasering of any external scars may improve final appearance.
- Resume all skin care, including facials/extractions/hydrofacials. Wear sunscreen.
Stage 4: Three months to one year after surgery
- Swelling: Firmness/ numbness will gradually subside, though typically your nose will always be more firm than before surgery due to structural grafting.
- Long term, the skin and soft tissues of the nose continue to thin down. Sometimes irregularities to appear as this happens. Although it is commonly said that the nose is all healed after one year, this may not be the case after revision rhinoplasty. Two or three years may be required for full softening of the tissues. Episodes of swelling that appear, then disappear a day later, are common and gradually become less and less. Until they resolve completely, you are still healing.
When will I know if I need yet another revision rhinoplasty?
Once the initial swelling has improved, both the shape and the function of the nose can be assessed. With revision rhinoplasty, this can take quite some time. If there is still a significant problem after 9 months of recovery, it is worth bringing up your concerns with your surgeon.
How much does revision rhinoplasty cost?
Costs of revision rhinoplasty vary significantly from state to state, and even from city to city within a state. Here in Texas, for example, revision rhinoplasty can cost twice as much in Dallas as it does in Austin for the same surgery by a surgeon of equal experience. Things that add to the cost are how difficult your particular surgery is, how many previous surgeries you have had, if the problem is cosmetic, functional or both, and how experienced your surgeon is. If ear or rib cartilage is required, then costs will be more. Length of surgery will also increase the cost, since more time is required for anesthesia and facility fees.
A summary of rhinoplasty costs can be found in our blog article “Cosmetic Procedure Cost Guide”. Revision rhinoplasty costs are typically 30% to 100% higher than primary rhinoplasty costs in most areas of the country.
How do I find the best revision rhinoplasty surgeon in my area?
There are minimum standards your surgeon should achieve to refer to themself as a rhinoplasty surgeon. First, he/she should be either a board-certified plastic surgeon or a board-certified facial plastic surgeon. These are distinct but parallel means that guarantee a minimum level of training and standard of care.
- American Board of Facial Plastic & Reconstructive Surgery (ABFPRS): Board certification requires certification by an American Board of Medical Specialties (ABMS) board first [either American Board of Otolaryngology (ABOto) or American Board of Plastic Surgery (ABPS)]. Then, the candidate surgeon must pass a written and oral board examination and present a minimum number of cases in facial plastic surgery over a 2-year interval. This Board focuses only on facial plastic surgery.
- American Board of Plastic Surgery (ABPS): This is an ABMS board. A surgeon must complete a written and oral examination and present a certain number of plastic surgery cases he has performed. This Board focuses on plastic surgery of the face, body and hands.
In addition to selecting a board-certified surgeon, the physician you choose should demonstrate excellence in rhinoplasty in general and in revision rhinoplasty in particular. Being competent in rhinoplasty alone does not guarantee competence in revision rhinoplasty. The surgeon can demonstrate that he or she is a revision rhinoplasty expert by presenting at national/ international meetings, publishing in scientific, peer-reviewed journals, being a teacher/mentor to younger surgeons/residents, and showing superior results in presentations to patients and on their website.
To see the credentials of our surgeons at Westlake Dermatology, please visit our Physicians page and click on each surgeon.
To see before-and-after pictures from our surgeons, please visit our Revision Rhinoplasty Gallery.
 Before
Before  After
After  Before
Before 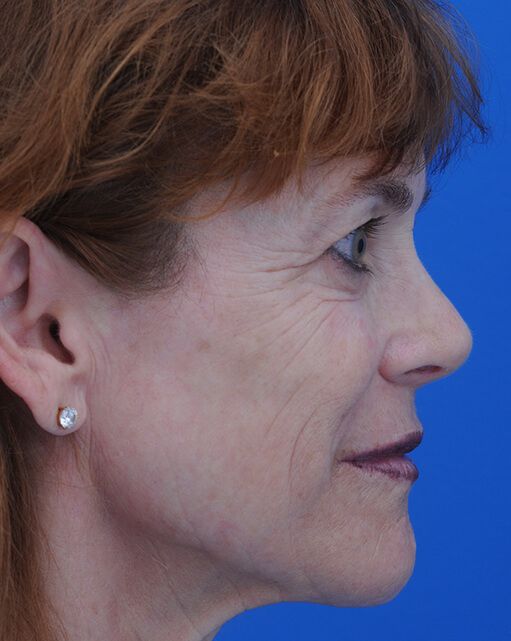 After
After