

Rhinoplasty
Rhinoplasty is a surgical procedure that changes the shape of the nose to improve the whole face. Rhinoplasty can be cosmetic, functional or both.
WHAT IS RHINOPLASTY?
A subtle change to the nose can impact the appearance of an entire face. Rhinoplasty, or nose surgery, can be performed to alter the natural shape of the nose, or correct the appearance that may have been altered from an injury or during prior surgery.
The goal of rhinoplasty is not to create the perfect nose, but rather to improve how your nose fits your face. By making the nose match the face better, the aesthetic of the entire face is more balanced and improved. Your eyes will be more captivating. Your smile will be brighter. Rhinoplasty can create subtle change or dramatic change, depending on how disproportionate your nose is to begin with.
Before and After Rhinoplasty
View Rhinoplasty Photo Gallery
DO I NEED A RHINOPLASTY?
The answers to these questions can help determine if rhinoplasty is right for you:
- Does your nose interfere with how your eyes and smile appear because of its size (too big, too small) or position (too long, crooked)?
- Do you have nasal obstruction, or have you ever had a nasal fracture?
If the answer to #1 is “Yes”, then you are a candidate for Cosmetic Rhinoplasty. If the answer to #1 is “Yes” and the answer to #2 is “Yes”, then you may be a candidate for Functional Rhinoplasty.
HOW IS RHINOPLASTY PERFORMED?
Rhinoplasty is surgery tailored to an individual patient’s particular needs. The surgery is comprised of the approach, the technique and the closure. No two rhinoplasties are the same, making it the most creative and the most challenging plastic surgery performed on the face.
Approach: The approach is how the surgeon actually gets to the parts of the nose to be operated on.
- Open (external) approach: The open approach is the most commonly used approach today. Introduced in the early 1980’s to the U.S., it gradually increased in popularity until it became the most popular approach by the 1990’s. It involves making an incision in the columella (the area between the nostrils) and connecting it with incisions inside the nostril edges (marginal incisions). Through these incisions the skin is raised off the underlying cartilages and bones so the surgeon can execute their chosen technique. Septoplasty and nasal valve surgery can both be performed through this approach and do not require separate incisions.
- Endonasal (closed) approach: While not used as commonly as the open approach, the endonasal approach involves making two parallel incisions inside the nose. The first is the same marginal incision as the open approach along the edges of the nostrils. The second is higher, where the top of the tip cartilages meet the sidewall cartilages (upper lateral cartilages), and is called an intercartilagenous incision. Through these incisions the surgeon can access the tip cartilages and the top of the nose. Typically, a separate incision is made to access the septum. The endonasal approach is reserved for smaller surgeries such as nasal fracture repairs where no tip work, nasal valve work or severe deviations need to be corrected.
Technique: What the rhinoplasty surgeon does to change nasal shape and function.
- Tip refinement: The nasal tip can be narrowed, straightened and refined by rotating or counter-rotating it, or projecting or de-projecting it. Old-style techniques relied on removing cartilage to create narrowing. However, the modern rhinoplasty surgeon knows that removing too much cartilage will lead to undesired changes in the years to come. Instead, today the tip is refined by repositioning and bending nascent cartilages, then adding structural stability using cartilage grafts from the septum. This creates a stable, strong tip that can maintain its position over a lifetime.
- Dorsum changes: The dorsum, also known as the nasal ridge, can be lowered by removing bone and cartilage. We preserve the upper lateral cartilages when we lower dorsal humps since they are critical to maintaining normal nasal airflow through the internal nasal valves. Often, invisible grafts, called spreader grafts, are placed to stabilize this area and to correct deviations.
- Preservation rhinoplasty: This technique, originating in the 1950’s, has seen a resurgence amongst rhinoplasty surgeons abroad in the past 5-10 years. It relies on changing the base of the nasal bones and septum to lower dorsal humps, leaving the bones and cartilages of the dorsum intact. The technique is still being developed so has not been embraced by most U.S. rhinoplasty surgeons yet.
- Nasal bones: 95% of all rhinoplasties require the nasal bones to be “broken”. This is because immediately after a hump is removed, the dorsum is flat. The nasal bones have to be precisely cut at their bases to move them inwards, recreating a smooth, rounded bridge. If this critical step is not performed, an “open roof deformity” occurs, which has an unnatural appearance. If the nose is crooked, the nasal bones are cut as part of the straightening process.
- Septoplasty: A surgical procedure to straighten the septum (the bone and cartilage dividing the space between the nostrils) is often required in conjunction with rhinoplasty. Even when no breathing problem is present, septal cartilage is often used for grafting. Many patients also have septoplasty to improve their breathing at the same time as rhinoplasty.
- Nasal valve surgery: The nasal valves are the narrowest parts of the nose and regulate nasal airflow. Valve surgery to improve or maintain nasal airflow defines “functional rhinoplasty”.
- Alar base surgery: Overly wide nostrils can be narrowed with surgery at the base of the nostrils. Alar base narrowing is accomplished using incisions around the nostrils. When large tips are de-projected to make them smaller, the nostrils may end up flaring. Alar base surgery can improve the flare so the whole tip looks better.
Closure: Once rhinoplasty is completed the incisions must be closed.
- Sutures: External incisions are closed using sutures that are removed 5 to 7 days after surgery. Internal incisions are closed with sutures that dissolve on their own after 7 to 21 days.
- Internal splints: Septal splints come in all shapes and sizes. When needed, thin sheets of rubber are sewn along the septum to stabilize it for the first week of healing.
- Packing: A small amount of packing is placed into the nose at the end of the surgery and is removed as soon as you are fully awake in the recovery room. Packing is not left in place overnight since it can lead to increased pain, claustrophobia and increased infection risk.
- Cast: A cast is always placed for one week to stabilize the nose and limit swelling.
Video: Rhinoplasty Case Study
HOW DO I PREPARE MYSELF FOR RHINOPLASTY?
- Stop smoking: Smoking impairs the microcirculation in the skin, causing an increased risk of scarring, infection, and prolonged swelling. It also impairs the natural function of the nasal lining, so normal breathing and sinus function takes much longer to return. All nicotine products, including vaping, must be stopped for at least one month before and after surgery.
- Control your acne: Acne typically worsens for three months post-op, so it’s wise to get it under control prior to surgery.
- Maintain diet: A high protein, low carb diet can prime your body for healing. Caffeine may alter the microcirculation in the nose. Milk products can thicken your secretions.
- Lymphatic massage: This can open your lymphatics and shorten your swelling after surgery. It is even more beneficial if performed prior to your surgery.
- Arnica montana: This homeopathic herb can shorten how long your bruising lasts after rhinoplasty.
- Mupirocin ointment: Using this prescription antibiotic ointment intranasally for one week before surgery can reduce your risk of infection by MRSA (methicillin-resistant Staph aureus).
- Prophylax against herpes: If you are prone to cold sores or herpes around the mouth and nose, speak to your surgeon about taking prophylactic anti-viral medication before your surgery.
- Hydrate: Surgery and general anesthesia are dehydrating. Coming into the operating room well-hydrated will make you feel better faster, with less postoperative nausea. You will not be able to eat or drink anything from midnight the night before surgery, so begin hydrating at least three days prior to your surgery.
- Use sunscreen: If you come into surgery with your nose sunburned, your risk of infection and swelling increases.
WHAT IS THE HEALING PROCESS FROM THE RHINOPLASTY?
Although it takes a full year to completely heal from any surgery, most of the healing after rhinoplasty is completed in three months.
- Immediately after surgery through 7 days: During the first overnight period there is bleeding. The moustache dressing under your nose may get soaked through every 30 minutes after you get home from surgery. Usually bleeding slows down and stops by the next morning. Use ice and keep your head elevated to help minimize the swelling and bruising, which typically peaks at 48 to 72 hours after surgery. Internal swelling causes severe nasal obstruction. External swelling makes the tip turn up and the upper lip swell.Pain is managed with a combination of ice, celeoxib (Celebrex) and narcotic. Pain typically subsides after the second night, but it is common to need some narcotic until then, especially at night. Minimize any exertion during this time and continue the treatments you started to prepare for rhinoplasty.
- One week to one month: After one week the cast and stitches are removed. Swelling begins to significantly subside and breathing improves. At this point the nose still looks upturned and your smile feels stiff until after the second week, when things start to settle more quickly. Warm compresses may be started on the bruising to help it resolve faster, if still present. Lymphatic massage can help reduce swelling. You may be asked to tape your nose at night if your swelling is severe. You may wear eyeglasses as long as they don’t hurt, and you may begin exercise after the second week. You may gently blow your nose, get the nose wet, and after the second week you may swim but avoid wearing goggles. Protect your nose from getting sunburned. Your nose is still not stable enough to withstand getting hit, so be careful.
- One month to three months: Swelling rapidly subsides during this period, but your nose still feels very hard and numb. Your smile has returned to normal. After two months, you can resume recreational sports. If your nose gets hit it should be able to withstand the injury (unless it is a hard blow, so use caution). If your swelling is persisting too long, then lymphatic massage, taping at night and steroid injections can help it come down faster.
- Three months to one year: The firmness and numbness of your nose improves in most patients by one year, but in patients with thicker skin it may persist even longer.
Dr. Constantinides Discusses Rhinoplasty on KVUE News
RISKS AND COMPLICATIONS OF RHINOPLASTY
There are short-term risks and long-term risks of rhinoplasty. Short term risks include infection, severe bleeding, hematoma and risks of general anesthesia. Long term risks include poor outcome aesthetically, continued nasal obstruction and scarring.
Try to get an estimate from your surgeon of what your chances are for a good result and if there are any particular challenges with your rhinoplasty. The more obstructed, disproportionate, or deviated your nose is, the harder it is to get an excellent result.
WHAT IS REVISION RHINOPLASTY?
Revision rhinoplasty is additional surgery determined to be needed following a primary (initial) rhinoplasty. Revision can range from a little touch-up to a major redo. Revisions after primary rhinoplasty surgeries at Westlake Dermatology are less than 5%.
One year after your primary rhinoplasty is the time to look critically at your nose. Has it improved since preop condition? Is there still a breathing problem? Is there noticeable asymmetry? You and your surgeon may decide that a touch-up is needed to improve your nose further, though subjecting yourself to additional surgery for minimal gain should be carefully considered.
For a full discussion of revision rhinoplasty, please see our Revision Rhinoplasty page.
WHAT IS FUNCTIONAL RHINOPLASTY?
Functional rhinoplasty is a surgical procedure that is performed to correct various breathing constriction issues, with a secondary goal of enhancing the overall appearance of the nose.
Functional rhinoplasty techniques repair the nasal valves (the internal cartilage valves within the nostrils that regulate air flow) in order to restore proper breathing. The nasal valves can be congenitally narrow (from birth) or can collapse due to normal aging, injury or previous cosmetic rhinoplasty surgery. Functional rhinoplasty restores the nasal passageways to allow for normal functionality. While surgery on the nasal valves is usually performed to restore breathing, it can also enhance the appearance of the nose.
For a full discussion of functional rhinoplasty, please see our Functional Rhinoplasty page. Please note that functional rhinoplasty is only available at our Lamar Central location.
WHAT IS LIQUID RHINOPLASTY?
Liquid rhinoplasty is a non-surgical treatment performed by using fillers to change the shape of the nose. Results are not permanent. See our Liquid Rhinoplasty Blog for more information.
HOW MUCH DOES RHINOPLASTY COST?
The price of rhinoplasty varies between markets, experience level of your surgeon, and the patient’s individual surgical needs (such as if a septoplasty will be performed at the same time). For a precise quote at Westlake Dermatology, please select a surgeon you would like to consult with then schedule a consultation appointment.
For more information about the price of rhinoplasty and other plastic surgeries, visit our Rhinoplasty Cost Guide.
Rhinoplasty Webinar with Dr. Constantinides
PHOTO-IMAGING FOR RHINOPLASTY
Where available, photo-imaging is a useful tool to help you determine if rhinoplasty is right for you. By morphing photos to show changes in nasal length, rotation, projection and proportion, you and your surgeon can decide exactly what your goals are. In skilled hands, photo-imaging can predict with greater than 90% accuracy how your nose will look after surgery. Learn more about photo-imaging for rhinoplasty
HOW DO I FIND THE BEST SURGEON FOR ME?
These criteria might help you in your search for a surgeon that matches well with your goals and aesthetics:
- Board certified by the American Board of Facial Plastic & Reconstructive Surgery (ABFPRS) or the American Board of Plastic Surgery (ABPS). Check the websites of each to confirm your surgeon’s board-certification is active. All surgeons at Westlake Dermatology are either board-certified or board-eligible.
- Ask how many rhinoplasty procedures a surgeon has performed to determine their level of experience.
- View the surgeon’s before-and-after pictures. Do you like the visible results? Do the eyes and face look better after rhinoplasty? Remember that surgeons only post their best results online. If you do not care for them, then look elsewhere.
- Check other credentials. Is the surgeon active locally and/or nationally in professional societies? Does the surgeon present at scientific meetings on rhinoplasty? Does the surgeon teach and/or publish scientific articles about rhinoplasty? All these factors add to the big picture, though not all are required to make a superior rhinoplasty surgeon.
- Have an in-person consultation. Pick a surgeon that you can trust to guide you through the significant healing after rhinoplasty. You should share the same aesthetic goals.
Additional Rhinoplasty Resources
- Nose Reshaping Without Surgery: Which Issues Can Be Corrected?
- Rhinoplasty For Crooked Nose Correction
- Correcting a Bulbous Nose with Rhinoplasty
- Exercising After Rhinoplasty: What To Know
- Bruising After Rhinoplasty: What You Need to Know
- Cosmetic Rhinoplasty vs. Functional Rhinoplasty vs. Septoplasty
- Can I Wear Glasses After Rhinoplasty?
- How Common Is Revision Rhinoplasty?
- Surgical & Non-Surgical Options For Correcting A Crooked Nose
- 4 Common Reasons for Rhinoplasty
- Rhinoplasty Recovery: Tips + What To Expect
- Innovations in Functional Rhinoplasty: The Latera Implant
- Nostril Asymmetry And Alar Retraction After Rhinoplasty
- Adding Volume in Surgical and Non-surgical Rhinoplasty
- Male vs. Female Rhinoplasty – What’s The Difference?
- The Non-Surgical Nose Job: All About Liquid Rhinoplasty
- Can Rhinoplasty Correct A Deviated Septum?
- Open Rhinoplasty vs. Closed Rhinoplasty
- What is Ethnic Rhinoplasty?
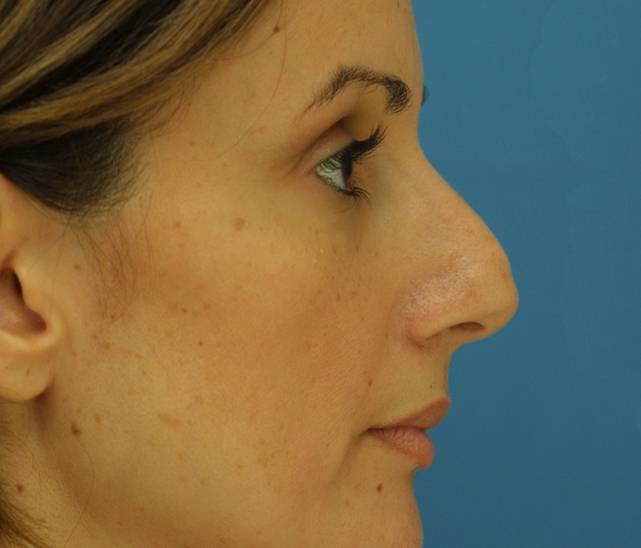 Before
Before 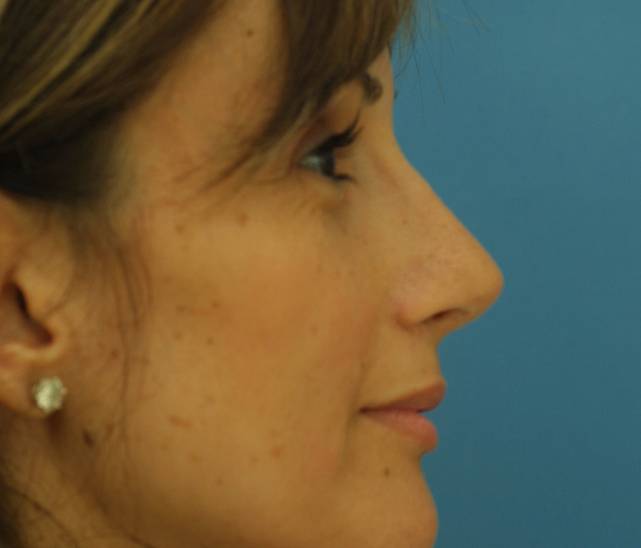 After
After  Before
Before 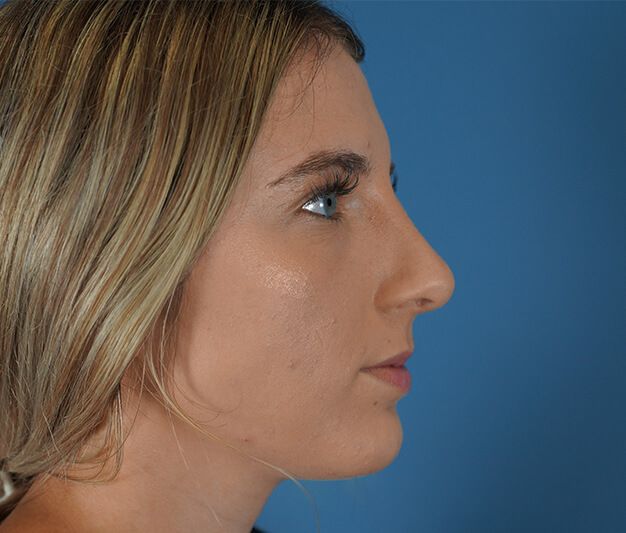 After
After 