Plaque Psoriasis Symptoms, Prevention, and Treatment Options
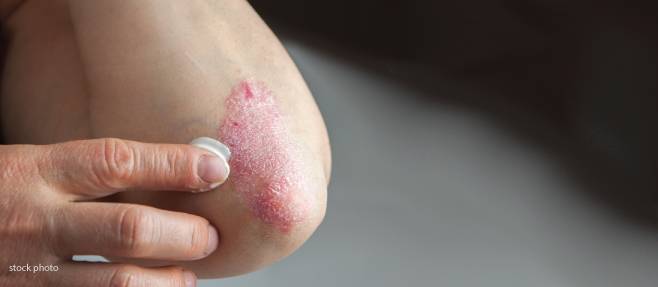
Studies show that approximately 3% of all adults have some form of psoriasis, a chronic skin condition that causes persistent itching, rashes, and scaling on the skin. Between 80% and 90% of people with psoriasis are diagnosed with plaque psoriasis, making it the most common type of psoriasis. Living with plaque psoriasis is challenging due to the physical and emotional effects of the condition. Unfortunately, there is no cure for plaque psoriasis. However, there are many effective treatment options to manage psoriasis by limiting the number and severity of symptom flare-ups.
What is Plaque Psoriasis?
Plaque psoriasis is a chronic condition that develops due to an over-production of skin cells. Healthy skin has the ability to shed dead skin cells as new cells form. In cases of plaque psoriasis, the body generates an overabundance of skin cells that are not shed. Over time, thick, scaly patches of skin form. Plaque psoriasis causes clusters and patches of scaly skin accompanied by itching, pain, and inflammation. The plaque typically has a silver-white appearance.
Types of Plaque Psoriasis
Plaque psoriasis is often categorized as small, large, unstable, or stable as follows:
- Small plaque psoriasis involves multiple, small lesions on the skin. Most of the lesions are less than a few centimeters in diameter. The clusters of lesions may remain separate or merge into larger clusters. The tops of the lesions tend to have a thin crust and pink color.
- Large plaque psoriasis involves clusters of thick, large lesions. The surfaces tend to be red with silvery-white scales.
- Unstable plaque psoriasis is described as lesions with undefined edges. The lesions tend to join to form larger patches of damaged skin.
- Stable plaque psoriasis involves persistent lesions that may disappear and then reappear with certain triggers.
What are the Symptoms of Plaque Psoriasis?
Patches of silver-white, scaly skin are the most common symptom of plaque psoriasis. Other symptoms may include pain, irritated skin, cracks in the skin, itching, and bleeding.
Where Does Plaque Psoriasis Occur on the Body?
Plaque psoriasis can appear on any part of the body, and it tends to be bilateral, meaning that it will appear in the same area on both sides of the body. Plaque development is most common on the knees, back, elbows, and scalp. People with severe cases of plaque psoriasis may develop lesions on their hands, feet, genitals, face, and legs.
What Causes Plaque Psoriasis?
Plaque psoriasis is caused by an autoimmune disorder in which the immune system overreacts to certain triggers. Although the exact mechanism of plaque psoriasis is not well-understood, the general belief is that infection-fighting cells in the body attack healthy skin cells. Known as leukocytes, the cells help the body defend against harmful substances. The leukocytes overstimulate the development of keratinocytes, the cells responsible for skin healing, and this forms the distinctive skin thickening of plaque psoriasis.
Are Certain People at Greater Risk for Plaque Psoriasis?
Researchers believe that environment, immune function, and genetics are the most likely contributing factors in determining the risk for plaque psoriasis. Environmental factors can include the individual’s emotional and physical experiences, such as stress, injuries, exposure to cold temperatures, certain infections, and alcohol and drug use. Some studies have revealed a possible connection between dental diseases and plaque psoriasis. Individuals who have a family history of plaque psoriasis are more prone to the condition.
While not a direct link, other commonalities among plaque psoriasis include:
- Being Caucasian
- Being overweight or obese
- Using tobacco and alcohol
- Experiencing episodes of depression and stress
- Failing to take (non-compliance with) certain medications
Can Plaque Psoriasis Be Prevented?
While plaque psoriasis cannot be prevented, there are take ways to reduce the frequency and severity of flare-ups. Triggers vary, and it is best to consult with a dermatologist to learn how to best manage your triggers.
Common Triggers for Plaque Psoriasis
Some of the more common triggers for plaque psoriasis flare-ups include:
- Weight Gain
- Stress
- Using alcohol or tobacco
- Certain types of infections and injuries to the skin
- Certain medications
- Changes to medication dosages
- Sun damage
- Dry skin
Once an individual understands their unique triggers, symptom flare-ups can through lifestyle changes focused on trigger avoidance.
Skin Care Tips for Plaque Psoriasis
There are steps that you can take to reduce flare-ups and protect your skin:
- The use of antihistamines may help with the itching.
- Avoid hot showers or baths. Instead opt for short, warm showers protect the skin barrier.
- Use a fragrance-free cream moisturizer daily and after bathing
- Use mild soaps that are made for sensitive skin.
- Soothe and calm your skin with a tar bath or Dead Sea salt.
- When you have a flare-up, wear loose clothing to allow your skin to breathe.
- Start an anti-inflammatory or Mediterranean diet and a turmeric supplement
Treatment Options for Plaque Psoriasis
Because plaque psoriasis is a chronic condition, the goal of treatment is to reduce symptoms. Effective treatment options for psoriasis include:
Topical Treatments
Various topical products such as tapinarof can be applied directly onto affected areas of the skin to bring local relief from plaque psoriasis. These topicals often contain ingredients like steroids, retinoids, calcipotriene and salicylic acid to help slow excess skin cell production or strip cells away.
Systemic Medications
Prescription medications like acitretin, aprimelast, methotrexate, or cyclosporine work by targeting a portion of the immune system that causes psoriasis.
Biologics
Whether injected or infused through IV, biologics work by blocking the activation of the cells that trigger the development of psoriasis. They target a specific portion of the immune system, which is responsible for both psoriasis and psoriatic arthritis development. Common biologics include Enbrel, Humira, Stelara, Cosentyx, Taltz, Skyrizi , Tremfya, and Illumya.
Phototherapy
Phototherapy, or light therapy, utilizes a narrow band ultraviolet B (NB UVB) light source to expose the skin to an exact amount of NB UVB to minimize psoriasis symptoms without causing damage to the skin. Phototherapy should be overseen by a board-certified dermatologist to ensure safety and efficacy.
Disclaimer: The contents of the Westlake Dermatology website, including text, graphics, and images, are for informational purposes only and are not intended to substitute for direct medical advice from your physician or other qualified professional.
