Nail Psoriasis: Symptoms, Causes, Prevention, and Treatment Options
What Is Nail Psoriasis?
Psoriasis is an inflammatory disease in which an overactive immune system causes epidermal cells to reproduce too quickly. While this typically causes red, scaly plaques on the skin, it can also lead to changes in nail color, texture, and shape. Nail psoriasis can cause discomfort or pain, making it difficult for people to use their fingers or toes. In extreme cases, people may have trouble standing or walking.
More than half those with skin psoriasis will eventually experience the condition on their nails. Of those with psoriatic arthritis, nearly 90% will eventually experience nail psoriasis.
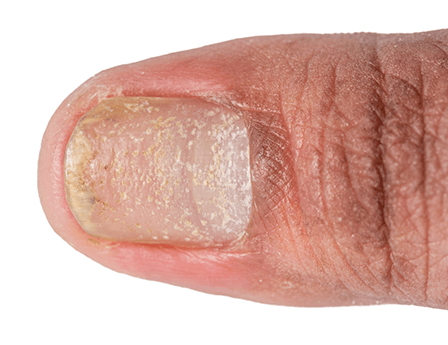
A close up of nail psoriasis
What Are The Symptoms Of Nail Psoriasis?
Nail psoriasis typically affects several fingernails, although it can be experienced on the toes. Symptoms include changes to the color, shape or texture of fingernails, such as the following:
- Discoloration: Nails may turn yellow, white or brown. There may be small reddish or brown spots or stripes under the nail, due to trapped blood.
- Pitting and Deformation: Small holes and other changes to the nail’s surface are common. Holes, ridges or grooves may be shallow or deep.
- Nail Thickening: Nails may appear thicker than normal as skin cells build up under the nail’s surface. Nail psoriasis may also trigger fungal infections which cause nails to thicken and become more brittle.
- Onycholysis: This is the separation of the nail from the nail bed. It can be painful and may lead to the nail’s disappearance over time.
Is It Nail Psoriasis or Nail Fungus?
Nail psoriasis is an inflammatory disease rather than an infection. However, the symptoms of nail psoriasis can increase your risk for a fungal infection.
If your dermatologist is unsure if your nail condition is the result of fungal infection or psoriasis, a small scraping or clipping can be taken to more closely to determine the cause. For this reason, we recommend that you do not clipping your nails right before your dermatology appointment.
Treatment can get rid of fungal infections, whereas there is no cure for nail psoriasis, only the mitigation of symptoms.
Who Is Most Susceptible To Developing Nail Psoriasis?
Most people who have experienced psoriasis of the skin or scalp will develop nail psoriasis. The condition typically appears on the nails several years after it has first appeared on the skin. In addition, the following factors seem to increase the risk for nail psoriasis:
- Being over 40 years old
- Being male at birth
- A family history of psoriasis or autoimmune disease
Are There Ways To Prevent Nail Psoriasis?
Nail psoriasis is a chronic condition. While it can go into remission with treatment, it cannot be cured. Flare-ups are always possible but can be minimized with good nail hygiene. Preventing damage to the nails can also help prevent flare ups.
- Keep nails short
- Wear protective gloves when working
- Keep nail edges filed and smooth
- Keep nails and cuticles well moisturized
- Wear shoes with plenty of comfortable space for your toes
- Avoid the use of caustic nail polishes, lacquers, gels or acrylics
When Should I See A Dermatologist?
If you haven’t been diagnosed with psoriasis and you notice a change in the appearance of your nails, it’s best to see your dermatologist. Your dermatologist can help you differentiate between nail psoriasis and an infection.
If you’ve been treating your nails for a fungal condition and you notice any of the following, contact your dermatologist:
- New symptoms or symptoms that aren’t improving with treatment
- Signs of infection, including irritation, swelling or discoloration
- Pain or the separation of nails from the nail bed
Since nail psoriasis is commonly associated with psoriatic arthritis, it’s best to get a diagnosis. Psoriatic Arthritis is a rheumatological condition that requires treatment.
Treatment Options for Nail Psoriasis
In general, the treatments for psoriasis are the same as those for nail psoriasis. Because the nails grow slowly, it may take 6 months or more to see cosmetic improvements. Stay consistent with whatever treatment you use before you decide it’s not working.
The treatment your dermatologist recommends will be based on the severity of your condition and where and how the nails are affected. Often, multiple treatments are used simultaneously to improve outcomes.
Treatments for nail psoriasis include the following:
- Topical Treatments: This may include the daily application of gels or creams, or the use of special medicated nail polish. These treatments apply corticosteroids directly to the nail or nail bed.
- Steroid Injections: In cases where topicals are not effective in reaching the nail bed, steroids may be injected. Prior to the injection, your dermatologist will numb the area. Treatments typically need to be repeated every 2-6 months.
- Phototherapy: Ultraviolet light is most effective for treating discoloration and nails that have begun separating from the nail bed. It is less effective at treating pitting or textural issues.
- Oral Medications: Systemic medications for the treatment of psoriasis may also reduce symptoms in the nails. These medications include Otezla (apremilast), Acitretin (Soriatane), Cyclosporine and Methotrexate.
- Injected Medications: Biologic or biosimilar drugs (such as Humira, Stelara, Cosentyx, Taltz, Skyrizi, or Tremfya) are given by injection and used to suppress specific functions of the immune system. They can help reduce the symptoms of psoriasis.
If your psoriasis has led to fungal infection as well, your dermatologist will recommend a treatment that can address the two simultaneously.
Disclaimer: The contents of the Westlake Dermatology website, including text, graphics, and images, are for informational purposes only and are not intended to substitute for direct medical advice from your physician or other qualified professional.

